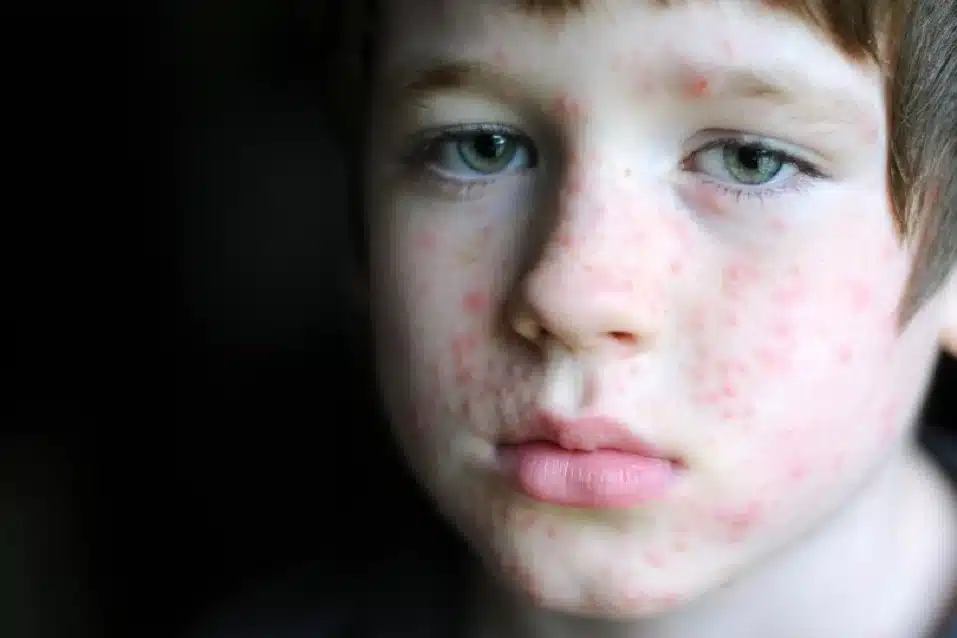
If a child or anyone in the family develops rashes that look like pimples or blisters, or have any other possible symptoms of monkeypox, they should contact their doctor immediately.
As the number of reported monkeypox cases and related deaths continue to rise globally, studies are underway to understand the epidemiology, sources of infection, and transmission patterns. Here are 10 things we know so far:
- The incubation period (interval from infection to onset of symptoms) of monkeypox can range from five to 21 days.
- Monkeypox causes fever, headache, backpain, muscle aches, lack of energy, swollen lymph nodes, and rashes. The rash begins as flat spots that turn into bumps, which then fill with fluid. These crust and fall off as they heal.
- Sometimes spots that look like pimples or blisters may develop before having any other symptoms. The rash tends to be more concentrated on the face and extremities rather than on the trunk.
- The monkeypox virus can spread from close contact with infected people or animals. One can become infected if they have direct contact with blood, bodily fluids, or fluid from the blisters; use bedding or other items contaminated by the virus; breathe in the virus.
- Transmission can also occur via the placenta from mother to foetus (congenital monkeypox) or during close contact during and after birth.
- Monkeypox is an orthopoxvirus, similar to the smallpox virus, but is less contagious and usually causes a milder disease.
- Usually, affected people, including children feel better within two to four weeks. However, in some cases, complications may arise, such as secondary infections, bronchopneumonia, sepsis, encephalitis, and infection of the cornea with ensuing loss of vision.
- Diagnosis of monkeypox is based primarily on clinical presentation. Lymph node enlargement during the early stage of illness can help distinguish monkeypox from chickenpox or smallpox.
- For conformation of the disease, polymerase chain reaction (PCR) can be performed on diagnostic samples from skin lesions – the roof or fluid from vesicles and pustules, and dry crusts. However, the tests are usually inconclusive because of the short duration of viraemia. Biopsy is another option.
- As with many microbes, washing hands well and often, masking, and avoiding contact with sick people and animals can help protect one from getting the infection.
Dealing with the infection in children
If a child or anyone else in the family develops rashes that look like pimples or blisters, or have any other possible symptoms of monkeypox, they should contact their doctor immediately. A sick child with uncontrolled fever or severe aches or significantly reduced activity may need urgent evaluation and care in a hospital.
Currently, there are no specific treatments for monkeypox virus infection. The symptoms often resolve on their own without the need for treatment, but symptomatic treatment may keep the affected children more comfortable.
Clinical care includes alleviation of symptoms, management of complications and prevention of long-term sequelae. Children often suffer from fever and sometimes, body aches, and hence medication for pain (analgesics) and fever (antipyretics) can be used to relieve these symptoms. It is also important to keep children well hydrated.
Affected children should be advised to wash their hands before and after touching the lesions and keep the skin dry and uncovered. In case, they are in a room with someone else, the lesions should be covered with clothing or a bandage until they are able to isolate again.
The rash can be kept clean with sterilised water or antiseptic. Saltwater rinses can be used for lesions in the mouth, and warm baths with baking soda and Epsom salts can help with lesions on the body. Lidocaine can be applied to oral and perianal lesions to relieve pain. Secondary bacterial infections, though, may need antibiotics.
Smallpox vaccines are effective against monkeypox infection, and a vaccine created to prevent both smallpox and monkeypox is available now, and may be introduced, should the need arise.
(The author is a consultant – Pediatrics and Neonatology, Cloudnine Group of Hospitals, Bengaluru, India.)